After the Affordable Care Act went into effect in January 2014, states had the option to expand Medicaid coverage to people whose incomes fall within 138 percent of the federal poverty level. To encourage states to expand their insurance coverage, Congress made the federal government responsible for paying most or all of the costs associated with the expansion through 2020. As a result, 36 states and the District of Columbia have expanded Medicaid. Not surprisingly, both enrollment and federal spending have increased in the past few years. In 2017, 73.8 million people were enrolled in Medicaid, up from 59.8 million in 2013. During the same time frame, spending grew from $495 billion to $592 billion.
In June 2018, the Centers for Medicare & Medicaid Services (CMS) launched a new five-year Medicaid program integrity strategy to control costs; ensure that state agencies correctly enroll people who are actually eligible under expanded coverage; and weed out new instances of waste, fraud, and abuse. As CMS announced, “with this historic growth comes an equally growing and urgent responsibility to ensure sound stewardship and oversight of our program resources.” Such program integrity efforts are important for making sure taxpayer-funded benefits and services go to only those who truly need them, which is critical for maintaining the public’s trust in government.
At the same time, having worked at a state Medicaid agency, I know how federal mandates can look and feel to those who have to comply with them: as another layer of red tape that states have no time for and that risks upsetting consumers and providers, impeding access to care, and diminishing the quality of services. It is virtually guaranteed to mean more federal oversight reviews and compliance audits, and it could potentially mean loss of revenue if CMS finds instances of improper payments, overpayments, or unallowable claims.
But the new plan from CMS does not have to be a headache for Medicaid agencies. States should look at the push from CMS as motivation to adopt a different model of program integrity, built on the concept of enterprise risk management (ERM), that will enable them to provide higher quality health care to more consumers in need while still meeting federal goals of cost containment, transparency, and accountability. They can also use the plan to build executive and legislative buy-in, pointing to federal expectations and thought leadership emphasizing the importance of program integrity. Lastly, they can use the plan as a guide to prioritize initiatives that provide the most value and have been deemed a high priority by their federal partners for program integrity.
Traditionally, program integrity in Medicaid has focused on fraud, waste, and abuse, a reactive approach overly reliant on chasing down bad actors after the improper payments had occurred. Instead, agencies should use proactive and preventive risk assessment techniques to avoid costs at the three front doors: provider screening, consumer eligibility, and financial management. With a proactive strategy to prevent improper payments, states will have more resources for developing new and innovative services. Mathematica is helping states adopt an approach that will enable them to pay for the right services to the right providers for the right consumers, the first time and every time after. After they do so, states can apply the same approach to other public assistance programs, such as the Supplemental Nutrition Assistance Program and Temporary Assistance for Needy Families, enabling state departments of health and human services to be more consistent and holistic in how they handle program integrity.
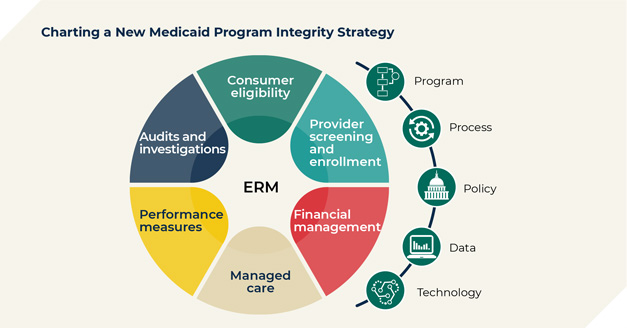
When Mathematica works with state Medicaid agencies looking to chart a new ERM strategy, we focus on three areas:
Context. States should tailor their strategy to their specific program, policies, and processes, which might entail risk assessments and other forms of analysis or review before they change their current approach to program integrity.
Technology. States must assess their budget constraints and specific operational needs before selecting the right technology for their ERM approach.
Data. ERM works best when data are timely, accurate, and complete. With high quality data, states can use machine learning, social network analysis, and other forms of data analytics or modeling to find and prevent overpayments on a continual basis.
Mathematica is excited to work with states as they make progress on more effectively providing Medicaid services while reducing or slowing program costs.


